Automatic O2 Control
Our award winning OxyGenie® module is a responsive Automatic O2 controller for the SLE6000.
Designed with the University of Tasmania and the Royal Hobart Hospital, SLE wanted to create a solution that
maximises the amount of time the patient’s SpO2 is within target range, by analysing their FiO2 every second.

Queen’s Award for Enterprise: Innovation 2021
In 2021 OxyGenie® was given the Queen’s Award for Enterprise: Innovation.
This automatic O2 controller can help reduce the time spent adjusting the ventilator, allowing staff to spend more time caring for the patient. This is key for the high workload medical staff caring for preterm infants often face.
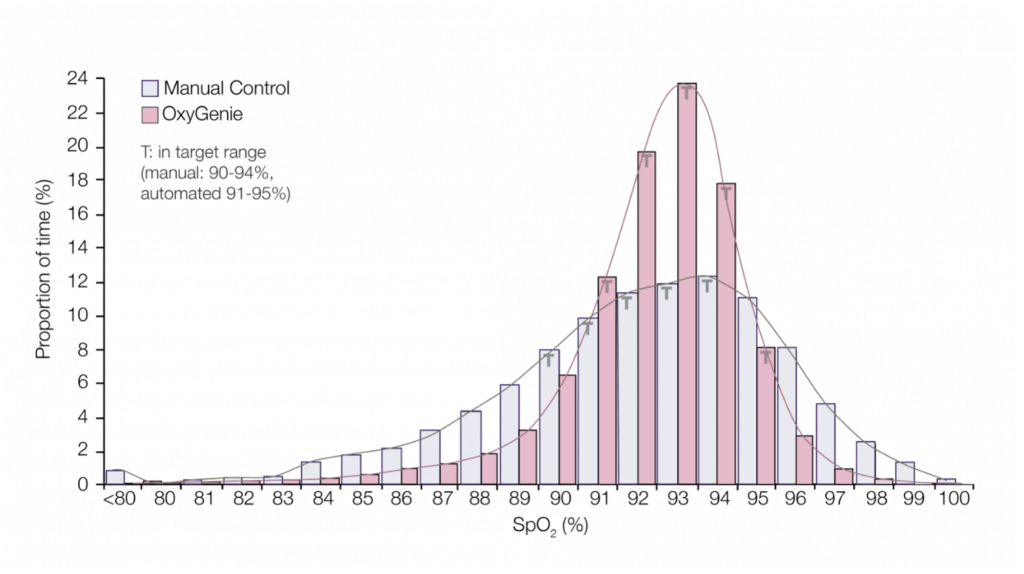
Manual Control VS Automatic Control
With the help of OxyGenie®, the patient’s FiO2 is automatically controlled, maximising the amount of time their SpO2 is within target range. OxyGenie® analyses the patient’s FiO2 every second and can make the necessary changes when there is a sudden change in a baby’s saturation.
Smooth integration with the SLE6000 & SLE1500
The algorithm incorporates additional software that has a different response depending upon the severity of lung disease, plus target range attenuation and Severinghaus compensation. The overall design of the software allows it to respond to both gradual and sudden changes in SpO2.

Search for Products
Please note, some products may not be available in your area. Please contact your local Sales Manager to find out more.
References:
Plottier GK, Wheeler KI, Ali SKM, Sadeghi Fathabadi O, Jayakar R, Gale TJ, Dargaville PA.
Clinical evaluation of a novel adaptive algorithm for automated control of oxygen therapy in preterm infants on non-invasive respiratory support.Arch Dis Child Fetal Neonatal Ed 2017; 102: F37-F43
https://pubmed.ncbi.nlm.nih.gov/27573518/
Education Hub
Online Training
Webinars
Service Training
Clinical Training




